Hispanic Women With Blood Pressure Issues During Pregnancy May Be at Risk for Later Heart Problems
[ad_1]
Hispanic women who developed signs of high blood pressure for the first time during pregnancy could be more likely to have problems with heart function and structure later in life, according to a study published in December 2023 in the journal Hypertension.
Conditions like preeclampsia, eclampsia, and gestational hypertension — known collectively as hypertensive disorders of pregnancy (HDP) — may be more closely linked to certain heart risks than regular high blood pressure, according to the authors.
On average, Hispanic women develop heart disease 10 years earlier than non-Hispanic women, according to the American Heart Association.
High blood pressure in pregnancy has lasting effects on heart health, says lead author Odayme Quesada, MD, cardiologist and medical director of the Women’s Heart Center at The Christ Hospital in Cincinnati. “Our study emphasizes the importance of early surveillance for hypertension and management in women whose pregnancy is complicated by hypertensive disorder of pregnancy to prevent later-life heart disease,” says Dr. Quesada.
According to Johanna Contreras, MD, advanced heart failure and transplant cardiologist at Mount Sinai Fuster Heart Hospital in New York City, “This study highlights why it’s important to perform research on diverse populations.” All populations have different risk factors, “and we now know that Hispanic and Black women have the highest maternal mortality [per the American Medical Association] due to cardiovascular diseases, so it’s important to screen these patients and create access to healthcare and preventive strategies,” says Dr. Contreras, who was not involved in the study.
Conditions Such as Preeclampsia and Gestational Hypertension Have More Than Doubled
Hypertensive disorders of pregnancy can cause problems during and after delivery and are a leading cause of maternal deaths, per Million Hearts.
According to research, the rate of hypertensive disorders of pregnancy more than doubled in the United States between 2007 and 2019, and the rate in Hispanic women reached more than 60 cases per 1,000 live births. Experts attribute the rise in cases to women being older at first pregnancy as well as the rise of being overweight and having obesity.
Changes in Heart Structure and Function
To explore a possible link between a history of hypertension during pregnancy with changes in cardiac structure and function (measured by an echocardiogram, a type of ultrasound scan) researchers recruited 5,168 Hispanic women taking part in the Hispanic Community Health Study–Study of Latinos, the largest study of the health of Hispanic and Latino adults in the United States.
The average age of the women was 59, and they had been pregnant at least once.
About 14 percent reported having high blood pressure for the first time while pregnant: 439 of them had gestational hypertension, 219 had preeclampsia, and 66 had eclampsia.
“We found that women with a history of pregnancy complicated by hypertensive disorder of pregnancy have alterations in how the heart contracts and relaxes, increased thickness of the heart wall, and higher rates of abnormal geometry in the left ventricle. This is important because all are known indicators of future cardiovascular disease and death,” says Quesada.
The anatomic abnormalities in systolic and diastolic function found in the study place those women in stage B heart failure, says Contreras. Systolic function is when the heart contracts to pump blood out, and diastolic is when the heart relaxes after contraction.
Research estimated that about 6.7 million people in the United States have heart failure (HF), and about 1 out of every 4 people will develop the chronic condition in their lifetime. There are four heart failure stages, and Cleveland Clinic notes stage B is considered pre–heart failure — it means the left ventricle isn’t working well or is structurally abnormal but there aren’t any symptoms yet.
Though previous studies have associated such pregnancy complications with an increased risk for cardiovascular disease and even death, these new findings suggest structural and functional changes in the heart may be what’s driving that increased risk, cites the study authors.
This study helps to clarify that, for some women, pregnancy is not just a “stress test” that unmasks underlying cardiovascular risks, says senior author Susan Cheng, MD, MPH, the Erika J. Glazer Chair in Women’s Cardiovascular Health and Population Science at Cedars-Sinai in Los Angeles. “This risk may also affect the heart years after pregnancy,” she adds.
In the ‘Real World,’ These Changes in Heart Structure Wouldn’t Be Found
Current guidelines call for the diagnosis and management of hypertensive disorders during pregnancy, but these findings suggest that it may be a good idea to consider performing echocardiograms in these patients, says Contreras.
Quesada agrees that physicians do not generally order heart ultrasounds for women unless they are showing signs or symptoms of heart disease.
“More research is needed to determine whether echocardiograms are warranted in symptom-free women who had high blood pressure during pregnancy to detect abnormalities that may need early treatment,” she says.
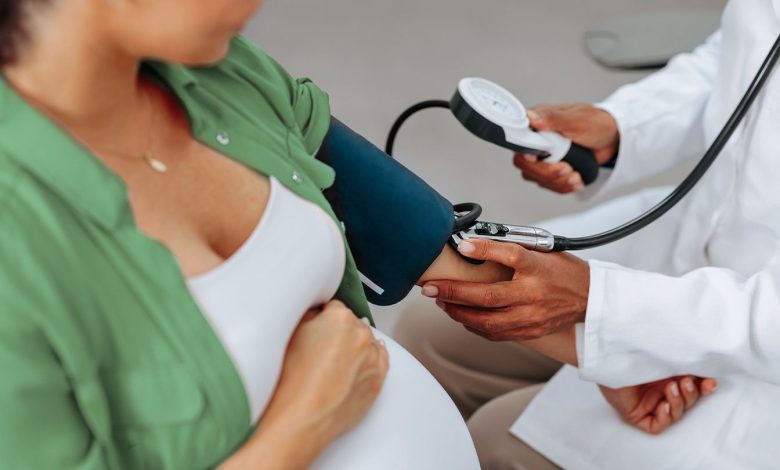
In the meantime, experts recommend monitoring blood pressure because it’s the key vital sign to detect hypertensive disorders in pregnancy. If it’s above 120/80 mmHG, tell your doctor or pharmacist.
Women can measure their blood pressure at a pharmacy or with a home blood pressure monitor, notes the Centers for Disease Control and Prevention. Your doctor can tell you how often to check and record your blood pressure readings. For some people, it might be a few times a week, and if you are at higher risk during pregnancy, you may need to do a reading twice a day, according to the Preeclampsia Foundation.
All women — pregnant or not — should have heart-health screenings regularly. Blood pressure should be measured at each regular healthcare visit or at least once per year if blood pressure is at or below optimal levels, according to the American Heart Association.
[ad_2]




